Health Management Solutions
For self-insured employers, the ideal would be to have more control over your employer-sponsored health care. We have created Populytics Health Management Solutions (PHMS), a direct-to-employer model, based on that concept. It gives you uncomplicated, efficient, cost-conservative health care coverage for your employees without the involvement of an insurance company.

Comprehensive Health Care
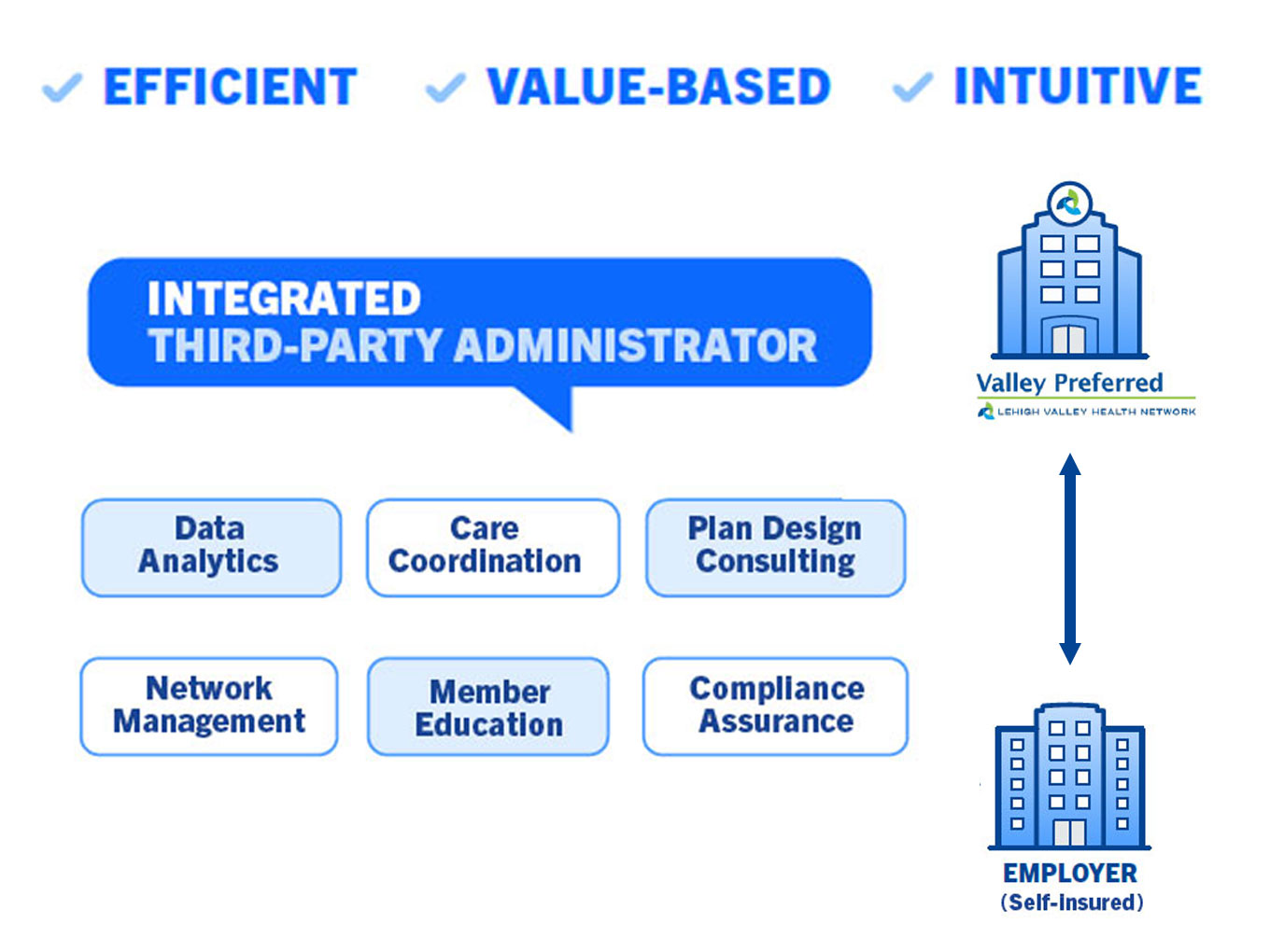
We apply all of our population health expertise while connecting you directly to clinicians dedicated to quality. Our platform spans health plan administration through data analytics, care coordination, and well-being, and includes the services of an integrated TPA. Few direct-to-employer providers offer this much.
Populytics Health Management Solutions encompasses:
-
Health Plan Administration
-
Plan Design and Consultation
-
Claims Adjudication
-
Population Health Management, including analytics and informatics, care coordination, utilization management, pharmacy management, and physical and emotional well-being
-
Network Access Design
What Makes Us Different?
We put the focus on total cost-of-care for your employee population and provide the infrastructure and competencies to address each aspect.
- A close relationship with Lehigh Valley Health Network (LVHN), one of the largest hospital networks in Pennsylvania, and its thousands of top-tier health providers across the state
- Customized plan design flexibility
- Transparency into costs and quality
- Enhanced patient relationships through direct involvement with connected providers
- Predictive modeling to transform clinical health care data and claims information into actionable information for healthier populations
- Data-informed care coordination for closing gaps in employee care
Pop Health Hub
In depth conversation about Population Health Management with Dr. David Nash, Founding Dean Emeritus, Thomas Jefferson University, College of Population Health

A Guide to Populytics Health Management Solutions
Gain leverage over your company's health care expenditure with a direct connection to clinicians dedicated to quality.
Modal Window Content: